

lingzhong
第1楼2009/05/28
Establishment of Clean Room Classifications
The design and construction of clean rooms and controlled environments are covered in Federal Standard 209E. This standard of air cleanliness is defined by the absolute concentration of airborne particles. Methods used for the assignment of air classification of controlled environments and for monitoring of airborne particulates are included. This federal document only applies to airborne particulates within a controlled environment and is not intended to characterize the viable or nonviable nature of the particles.
The application of Federal Standard 209E to clean rooms and other controlled environments in the pharmaceutical industry has been used by manufacturers of clean rooms to provide a specification for building, commissioning, and maintaining these facilities. However, data available in the pharmaceutical industry provide no scientific agreement on a relationship between the number of nonviable particulates and the concentration of viable microorganisms.
The criticality of the number of nonviable particulates in the electronic industry makes the application of Federal Standard 209E a necessity, while the pharmaceutical industry has a greater concern for viable particulates (i.e., microorganisms) rather than total particulates as specified in Federal Standard 209E. A definite concern for counts of total particulates in injectable products exists in the pharmaceutical industry (see Particulate Matter in Injections 788 ).
The rationale that the fewer particulates present in a clean room, the less likely it is that airborne microorganisms will be present is accepted and can provide pharmaceutical manufacturers and builders of clean rooms and other controlled environments with engineering standards in establishing a properly functioning facility.
Federal Standard 209E, as applied in the pharmaceutical industry is based on limits of all particles with sizes equal to or larger than 0.5 µm. Table 1 describes Airborne Particulate Cleanliness Classes in Federal Standard 209E as adapted to the pharmaceutical industry. The pharmaceutical industry deals with Class M3.5 and above. Class M1 and M3 relate to the electronic industry and are shown in Table 1 for comparison purposes. It is generally accepted that if fewer particulates are present in an operational clean room or other controlled environment, the microbial count under operational conditions will be less, provided that there are no changes in airflow, temperature, and humidity. Clean rooms are maintained under a state of operational control on the basis of dynamic (operational) data.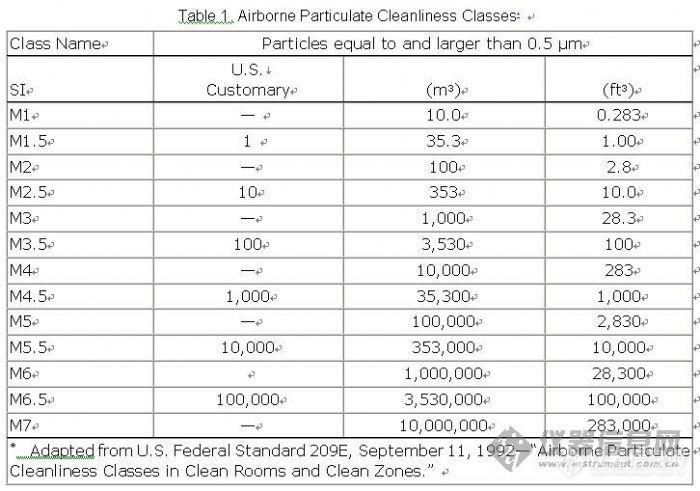
lingzhong
第2楼2009/05/28
Importance of a Microbiological Evaluation Program for Controlled Environments
Monitoring of total particulate count in controlled environments, even with the use of electronic instrumentation on a continuous basis, does not provide information on the microbiological content of the environment. The basic limitation of particulate counters is that they measure particles of 0.5 µm or larger. While airborne microorganisms are not free-floating or single cells, they frequently associate with particles of 10 to 20 µm. Particulate counts as well as microbial counts within controlled environments vary with the sampling location and the activities being conducted during sampling. Monitoring the environment for nonviable particulates and microorganisms is an important control function because they both are important in achieving product compendial requirements for Particulate Matter and Sterility under Injections 1 .
Microbial monitoring programs for controlled environments should assess the effectiveness of cleaning and sanitization practices by and of personnel that could have an impact on the bioburden of the controlled environment. Microbial monitoring, regardless of how sophisticated the system may be, will not and need not identify and quantitate all microbial contaminants present in these controlled environments. However, routine microbial monitoring should provide sufficient information to ascertain that the controlled environment is operating within an adequate state of control.
Environmental microbial monitoring and analysis of data by qualified personnel will permit the status of control to be maintained in clean rooms and other controlled environments. The environment should be sampled during normal operations to allow for the collection of meaningful data. Microbial sampling should occur when materials are in the area, processing activities are ongoing, and a full complement of operating personnel is on site.
Microbial monitoring of clean rooms and some other controlled environments, when appropriate, should include quantitation of the microbial content of room air, compressor air that enters the critical area, surfaces, equipment, sanitization containers, floors, walls, and personnel garments (e.g., gowns and gloves). The objective of the microbial monitoring program is to obtain representative estimates of bioburden of the environment. When data are compiled and analyzed, any trends should be evaluated by trained personnel. While it is important to review environmental results on the basis of recommended and specified frequency, it is also critical to review results over extended periods to determine whether trends are present. Trends can be visualized through the construction of statistical control charts that include alert and action levels. The microbial control of controlled environments can be assessed, in part, on the basis of these trend data. Periodic reports or summaries should be issued to alert the responsible manager.
When the specified microbial level of a controlled environment is exceeded, a documentation review and investigation should occur. There may be differences in the details of the investigation, depending on the type and processing of the product manufactured in the room. Investigation should include a review of area maintenance documentation; sanitization documentation; the inherent physical or operational parameters, such as changes in environmental temperature and relative humidity; and the training status of personnel involved. Following the investigation, actions taken may include reinforcement of training of personnel to emphasize the microbial control of the environment; additional sampling at increased frequency; additional sanitization; additional product testing; identification of the microbial contaminant and its possible source; and an evaluation of the need to reassess the current standard operating procedures and to revalidate them, if necessary.
Based on the review of the investigation and testing results, the significance of the microbial level being exceeded and the acceptability of the operations or products processed under that condition may be ascertained. Any investigation and the rationale for the course of action should be documented and included as part of the overall quality management system.
A controlled environment such as a clean zone or clean room is defined by certification according to a relevant clean room operational standard. Parameters that are evaluated include filter integrity, air velocity, air patterns, air changes, and pressure differentials. These parameters can affect the microbiological bioburden of the clean room operation. The design, construction, and operation of clean rooms varies greatly, making it difficult to generalize requirements for these parameters. An example of a method for conducting a particulate challenge test to the system by increasing the ambient particle concentration in the vicinity of critical work areas and equipment has been developed by Ljungquist and Reinmuller.1 First, smoke generation allows the air movements to be visualized throughout a clean room or a controlled environment. The presence of vortices or turbulent zones can be visualized, and the airflow pattern may be fine-tuned to eliminate or minimize undesirable effects. Then, particulate matter is generated close to the critical zone and sterile field. This evaluation is done under simulated production conditions, but with equipment and personnel in place.
Proper testing and optimization of the physical characteristics of the clean room or controlled environment is essential prior to completion of the validation of the microbiological monitoring program. Assurance that the controlled environment is operating adequately and according to its engineering specifications will give a higher assurance that the bioburden of the environment will be appropriate for aseptic processing. These tests should be repeated during routine certification of the clean room or controlled environment and whenever changes made to the operation, such as personnel flow, processing, operation, material flow, air-handling systems, or equipment layout, are determined to be significant.
lingzhong
第3楼2009/05/28
Training of Personnel
Aseptically processed products require manufacturers to pay close attention to detail and to maintain rigorous discipline and strict supervision of personnel in order to maintain the level of environmental quality appropriate for the sterility assurance of the final product.
Training of all personnel working in controlled environments is critical. This training is equally important for personnel responsible for the microbial monitoring program, where contamination of the clean working area could inadvertently occur during microbial sampling. In highly automated operations, the monitoring personnel may be the employees who have the most direct contact with the critical zones within the processing area. Monitoring of personnel should be conducted before or after working in the processing area.
Microbiological sampling has the potential to contribute to microbial contamination due to inappropriate sampling techniques. A formal personnel training program is required to minimize this risk. This formal training should be documented for all personnel entering controlled environments.
Management of the facility must assure that all personnel involved in operations in clean rooms and controlled environments are well versed in relevant microbiological principles. The training should include instruction on the basic principles of aseptic processing and the relationship of manufacturing and handling procedures to potential sources of product contamination. This training should include instruction on the basic principles of microbiology, microbial physiology, disinfection and sanitation, media selection and preparation, taxonomy, and sterilization as required by the nature of personnel involvement in aseptic processing. Personnel involved in microbial identification will require specialized training on required laboratory methods. Additional training on the management of the environmental data collected must be provided to personnel. Knowledge and understanding of applicable standard operating procedures is critical, especially those standard operating procedures relating to corrective measures that are taken when environmental conditions so dictate. Understanding of regulatory compliance policies and each individual's responsibilities with respect to good manufacturing practices (GMPs) should be an integral part of the training program as well as training in conducting investigations and in analyzing data.
The major source of microbial contamination of controlled environments is the personnel. Contamination can occur from the spreading of microorganisms by individuals, particularly those with active infections. Only healthy individuals should be permitted access to controlled environments.
These facts underscore the importance of good personal hygiene and a careful attention to detail in the aseptic gowning procedure used by personnel entering the controlled environment. Once these employees are properly gowned—including complete facial coverage—they must be careful to maintain the integrity of their gloves and suits at all times. Since the major threat of contamination of product being aseptically processed comes from the operating personnel, the control of microbial contamination associated with these personnel is one of the most important elements of the environmental control program.
The importance of thorough training of personnel working in controlled environments, including aseptic techniques, cannot be overemphasized. The environmental monitoring program, by itself, will not be able to detect all events in aseptic processing that could compromise the microbiological quality of the environment. Therefore, periodic media-fill or process simulation studies to revalidate the process are necessary to assure that the appropriate operating controls and training are effectively maintained.
lingzhong
第4楼2009/05/28
Critical Factors Involved in the Design and Implementation of a Microbiological Environmental Control Program
An environmental control program should be capable of detecting an adverse drift in microbiological conditions in a timely manner that would allow for meaningful and effective corrective actions. It is the responsibility of the manufacturer to develop, initiate, implement, and document such a microbial environmental monitoring program.
Although general recommendations for an environmental control program will be discussed, it is imperative that such a program be tailored to specific facilities and conditions. A general microbiological growth medium such as Soybean Casein Digest Medium should be suitable in most cases. This medium may be supplemented with additives to overcome or to minimize the effects of sanitizing agents, or of antibiotics if used or processed in these environments. The detection and quantitation of yeasts and molds should be considered. General mycological media, such as Sabouraud's, Modified Sabouraud's, or Inhibitory Mold Agar are acceptable. Other media that have been validated for promoting the growth of fungi, such as Soybean–Casein Digest Agar, can be used. In general, testing for obligatory anaerobes is not performed routinely. However, should conditions or investigations warrant, such as the identification of these organisms in sterility testing facilities, more frequent testing is indicated. The ability of the selected media to detect and quantitate these anaerobes or microaerophilic microorganisms should be evaluated.
The selection of time and incubation temperatures is made once the appropriate media have been selected. Typically, incubation temperatures in the 22.5 ± 2.5 and 32.5 ± 2.5 ranges have been used with an incubation time of 72 and 48 hours, respectively. Sterilization processes used to prepare growth media for the environmental program should be validated and, in addition, media should be examined for sterility and for growth promotion as indicated under Sterility Tests 71 . In addition, for the Growth Promotion test, representative microflora isolated from the controlled environment or ATCC strain preparations of these isolates may also be used to test media. Media must be able to support growth when inoculated with less than 100 colony-forming units (cfu) of the challenge organisms.
An appropriate environmental control program should include identification and evaluation of sampling sites and validation of methods for microbiological sampling of the environment.
The methods used for identification of isolates should be verified using indicator microorganisms (see Microbial Enumeration Tests 61 and Tests for Specified Microorganisms 62 ).
lingzhong
第5楼2009/05/28
Establishment of Sampling Plan and Sites
During initial start-up or commissioning of a clean room or other controlled environment, specific locations for air and surface sampling should be determined. Consideration should be given to the proximity to the product and whether air and surfaces might be in contact with a product or sensitive surfaces of container-closure systems. Such areas should be considered critical areas requiring more monitoring than non-product-contact areas. In a parenteral vial filling operation, areas of operation would typically include the container-closure supply, paths of opened containers, and other inanimate objects (e.g., fomites) that personnel routinely handle.
The frequency of sampling will depend on the criticality of specified sites and the subsequent treatment received by the product after it has been aseptically processed. Table 2 shows suggested frequencies of sampling in decreasing order of frequency of sampling and in relation to the criticality of the area of the controlled environment being sampled. 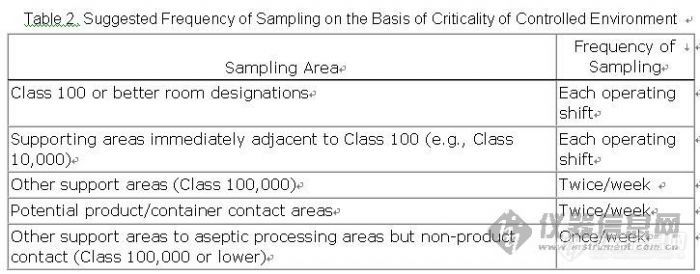
As manual interventions during operation increase, and as the potential for personnel contact with the product increases, the relative importance of an environmental monitoring program increases. Environmental monitoring is more critical for products that are aseptically processed than for products that are processed and then terminally sterilized. The determination and quantitation of microorganisms resistant to the subsequent sterilization treatment is more critical than the microbiological environmental monitoring of the surrounding manufacturing environments. If the terminal sterilization cycle is not based on the overkill cycle concept but on the bioburden prior to sterilization, the value of the bioburden program is critical.
The sampling plans should be dynamic with monitoring frequencies and sample plan locations adjusted based on trending performance. It is appropriate to increase or decrease sampling based on this performance.
lingzhong
第6楼2009/05/28
Establishment of Microbiological Alert and Action Levels in Controlled Environments
The principles and concepts of statistical process control are useful in establishing Alert and Action levels and in reacting to trends.
An Alert level in microbiological environmental monitoring is that level of microorganisms that shows a potential drift from normal operating conditions. Exceeding the Alert level is not necessarily grounds for definitive corrective action, but it should at least prompt a documented follow-up investigation that could include sampling plan modifications.
An Action level in microbiological environmental monitoring is that level of microorganisms that when exceeded requires immediate follow-up and, if necessary, corrective action.
Alert levels are usually based upon historical information gained from the routine operation of the process in a specific controlled environment.
In a new facility, these levels are generally based on prior experience from similar facilities and processes; and at least several weeks of data on microbial environmental levels should be evaluated to establish a baseline.
These levels are usually re-examined for appropriateness at an established frequency. When the historical data demonstrate improved conditions, these levels can be re-examined and changed to reflect the conditions. Trends that show a deterioration of the environmental quality require attention in determining the assignable cause and in instituting a corrective action plan to bring the conditions back to the expected ranges. However, an investigation should be implemented and an evaluation of the potential impact this has on a product should be made.
lingzhong
第7楼2009/05/28
Microbial Considerations and Action Levels for Controlled Environments
Classification of clean rooms and other controlled environments is based on Federal Standard 209E based on total particulate counts for these environments. The pharmaceutical and medical devices industries have generally adopted the classification of Class 100, Class 10,000, and Class 100,000, especially in terms of construction specifications for the facilities.
Although there is no direct relationship established between the 209E controlled environment classes and microbiological levels, the pharmaceutical industry has been using microbial levels corresponding to these classes for a number of years; and these levels have been those used for evaluation of current GMP compliance.2 These levels have been shown to be readily achievable with the current technology for controlled environments. There have been reports and concerns about differences in these values obtained using different sampling systems, media variability, and incubation temperatures. It should be recognized that, although no system is absolute, it can help in detecting changes, and thus trends, in environmental quality. The values shown in Tables 3, 4, and 5 represent individual test results and are suggested only as guides. Each manufacturer's data must be evaluated as part of an overall monitoring program. 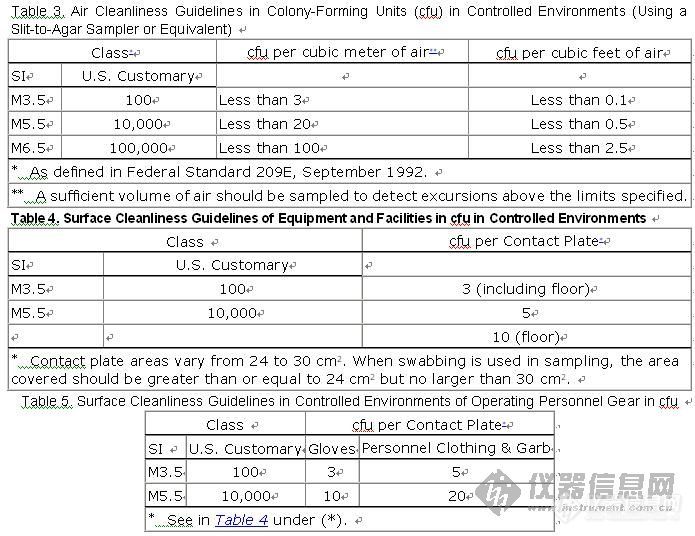
lingzhong
第8楼2009/05/28
Methodology and Instrumentation for Quantitation of Viable Airborne Microorganisms
It is generally accepted by scientists that airborne microorganisms in controlled environments can influence the microbiological quality of the intermediate or final products manufactured in these areas. Also, it generally is accepted that estimation of the airborne microorganisms can be affected by instruments and procedures used to perform these assays. Therefore, where alternative methods or equipment is used, the general equivalence of the results obtained should be ascertained. Advances in technology in the future are expected to bring innovations that would offer greater precision and sensitivity than the current available methodology and may justify a change in the absolute numbers of organisms that are detected.
Today, the most commonly used samplers in the U.S. pharmaceutical and medical device industry are the impaction and centrifugal samplers. A number of commercially available samplers are listed for informational purposes. The selection, appropriateness, and adequacy of using any particular sampler is the responsibility of the user.
Slit-to-Agar Air Sampler (STA)— This sampler is the instrument upon which the microbial guidelines given in Table 3 for the various controlled environments are based. The unit is powered by an attached source of controllable vacuum. The air intake is obtained through a standardized slit below which is placed a slowly revolving Petri dish containing a nutrient agar. Particles in the air that have sufficient mass impact on the agar surface and viable organisms are allowed to grow out. A remote air intake is often used to minimize disturbance of the laminar flow field.
Sieve Impactor— The apparatus consists of a container designed to accommodate a Petri dish containing a nutrient agar. The cover of the unit is perforated, with the perforations of a predetermined size. A vacuum pump draws a known volume of air through the cover, and the particles in the air containing microorganisms impact on the agar medium in the Petri dish. Some samplers are available with a cascaded series of containers containing perforations of decreasing size. These units allow for the determination of the distribution of the size ranges of particulates containing viable microorganisms, based on which size perforations admit the particles onto the agar plates.
Centrifugal Sampler— The unit consists of a propeller or turbine that pulls a known volume of air into the unit and then propels the air outward to impact on a tangentially placed nutrient agar strip set on a flexible plastic base.
Sterilizable Microbiological Atrium— The unit is a variant of the single-stage sieve impactor. The unit's cover contains uniformly spaced orifices approximately 0.25 inch in size. The base of the unit accommodates one Petri dish containing a nutrient agar. A vacuum pump controls the movement of air through the unit, and a multiple-unit control center as well as a remote sampling probe are available.
Surface Air System Sampler— This integrated unit consists of an entry section that accommodates an agar contact plate. Immediately behind the contact plate is a motor and turbine that pulls air through the unit's perforated cover over the agar contact plate and beyond the motor, where it is exhausted. Multiple mounted assemblies are also available.
Gelatin Filter Sampler— The unit consists of a vacuum pump with an extension hose terminating in a filter holder that can be located remotely in the critical space. The filter consists of random fibers of gelatin capable of retaining airborne microorganisms. After a specified exposure time, the filter is aseptically removed and dissolved in an appropriate diluent and then plated on an appropriate agar medium to estimate its microbial content.
Settling Plates— This method is still widely used as a simple and inexpensive way to qualitatively assess the environments over prolonged exposure times. The exposure of open agar-filled Petri dishes, or settling plates, is not to be used for quantitative estimations of the microbial contamination levels of critical enviroments.
One of the major limitations of mechanical air samplers is the limitation in sample size of air being sampled. Where the microbial level in the air of a controlled environment is expected to contain not more than three cfu per cubic meter, several cubic meters of air should be tested if results are to be assigned a reasonable level of precision and accuracy. Often this is not practical. To show that microbial counts present in the environment are not increasing over time, it might be necessary to extend the time of sampling to determine if the time of sampling is a limiting factor or not. Typically, slit-to-agar samplers have an 80-liter-per-minute sampling capacity (the capacity of the surface air system is somewhat higher). If one cubic meter of air is tested, then it would require an exposure time of 15 minutes. It may be necessary to use sampling times in excess of 15 minutes to obtain a representative environmental sample. Although there are samplers reported to be capable of very high sampling volume rates, consideration in these situations should be given to the potential for disruption of the airflow patterns in any critical area or to the creation of a turbulence that could increase the probability of contamination.
For centrifugal air samplers, a number of earlier studies showed that the samples demonstrated a selectivity for larger particles. The use of this type of sampler may have resulted in higher airborne counts than the other types of air samplers because of that inherent selectivity.
When selecting a centrifugal sampler, the effect of the sampler on the linearity of the airflow in the controlled zone where it is placed for sampling should be taken into consideration. Regardless of the type of sampler used, the use of a remote probe requires determining that the extra tubing does not have an adverse effect on the viable airborne count. This effect should either be eliminated or, if this is not possible, a correction factor should be introduced in the reporting of results.
lingzhong
第9楼2009/05/28
Methodology and Equipment for Sampling of Surfaces for Quantitation of Viable Microbial Contaminants in Controlled Environments
Another component of the microbial environmental control program in controlled environments is surface sampling of equipment, facilities, and personnel gear used in these environments. The standardization of surface sampling methods and procedures has not been as widely addressed in the pharmaceutical industry as the standardization of air sampling procedures.3 To minimize disruptions to critical operations, surface sampling is performed at the conclusion of operations. Surface sampling may be accomplished by the use of contact plates or by the swabbing method. Surface monitoring is generally performed on areas that come in contact with the product and on areas adjacent to those contact areas. Contact plates filled with nutrient agar are used when sampling regular or flat surfaces and are directly incubated at the appropriate time for a given incubation temperature for quantitation of viable counts. Specialized agar can be used for specific quantitation of fungi, spores, etc.
The swabbing method may be used for sampling of irregular surfaces, especially for equipment. Swabbing is used to supplement contact plates for regular surfaces. The swab is then placed in an appropriate diluent and the estimate of microbial count is done by plating of an appropriate aliquot on or in specified nutrient agar. The area to be swabbed is defined using a sterile template of appropriate size. In general, it is in the range of 24 to 30 cm2. The microbial estimates are reported per contact plate or per swab.
Culture Media and Diluents Used for Sampling or Quantitation of Microorganisms
The type of medium, liquid or solid, that is used for sampling or quantitation of microorganisms in controlled environments will depend on the procedure and equipment used. A commonly used all-purpose medium is Soybean–Casein Digest Agar when a solid medium is needed. Other media, liquid or solid, are listed below.
Liquid Media*
Solid Media*
Tryptone saline Soybean-casein digest agar
Peptone water Nutrient agar
Buffered saline Tryptone glucose extract agar
Buffered gelatin Lecithin agar
Enriched buffered gelatin Brain heart infusion agar
Brain heart infusion Contact plate agar
Soybean-casein medium
* Liquid and solid media are sterilized using a validated process.
These media are commercially available in dehydrated form. They are also available in ready-to-use form. When disinfectants or antibiotics are used in the controlled area, consideration should be given to using media with appropriate inactivating agents.
Alternative media to those listed can be used provided that they are validated for the purpose intended.
Identification of Microbial Isolates from the Environmental Control Program
The environmental control program includes an appropriate level of identification of the flora obtained from sampling. A knowledge of the normal flora in controlled environments aids in determining the usual microbial flora anticipated for the facility being monitored; evaluating the effectiveness of the cleaning and sanitization procedures, methods, and agents; and recovery methods. The information gathered by an identification program can also be useful in the investigation of the source of contamination, especially when the Action levels are exceeded.
Identification of isolates from critical areas and areas immediate to these critical areas should take precedence over identification of microorganisms from noncritical areas. Identification methods should be verified, and ready-to-use kits should be qualified for their intended purpose (see Critical Factors Involved in the Design and Implementation of Environmental Control Program).
lingzhong
第10楼2009/05/28
Operational Evaluation of the Microbiological Status of Aseptically Filled Products in Clean Rooms and Other Controlled Environments
The controlled environment is monitored through an appropriate environmental monitoring program. To assure that minimal bioburden is achieved, additional information on the evaluation of the microbiological status of the controlled environment can be obtained by the use of media fills. An acceptable media fill shows that a successful simulated product run can be conducted on the manufacturing line at that point in time. However, other factors are important, such as appropriate construction of facilities, environmental monitoring and training of personnel.
When an aseptic process is developed and installed, it is generally necessary to qualify the microbiological status of the process by running at least three successful consecutive media fills. A media fill utilizes growth medium in lieu of products to detect the growth of microorganisms. Issues in the development of a media fill program that should be considered are the following: media-fill procedures, media selection, fill volume, incubation, time and temperature, inspection of filled units, documentation, interpretation of results, and possible corrective actions required.
Since a media fill is designed to simulate aseptic processing of a specified product, it is important that conditions during a normal product run are in effect during the media fill. This includes the full complement of personnel and all the processing steps and materials that constitute a normal production run. During the conduct of media fill, various predocumented interventions that are known to occur during actual product runs should be planned (e.g., changing filling needles, fixing component jams).
Alternatively, in order to add a safety margin, a combination of possible conditions can be used. Examples may include frequent start and stop sequences, unexpected repair of processing system, replacement of filters, etc. The qualification of an aseptic process need not be done for every product, but should be done for each processing line. Since the geometry of the container (size as well as opening of the container) and the speed of the line are factors that are variable in the use of an aseptic processing line, appropriate combination of these factors, preferably at the extremes, should be used in the qualification of the line. A rationale for products used should be documented.
The 1987 FDA Guideline on Sterile Drug Products Produced by Aseptic Processing indicates that media-fill runs be done to cover all production shifts for line/product/container combinations. This guideline should be considered not only for qualification media-fill runs, but also for periodic reevaluation or revalidation. Media fill programs should also simulate production practices over extended runs. This can be accomplished by doing media-fill runs at the end of production runs.
In general, an all-purpose, rich medium such as Soybean Casein Broth that has been checked for growth promotion with a battery of indicator organisms (see Sterility Tests 71 ) at a level of below 100 cfu/unit, can be used. Isolates from the controlled environment where aseptic processing is to be conducted may also be used. Following the aseptic processing of the medium, the filled containers are incubated at 22.5 ± 2.5 or at 32.5 ± 2.5 . All media filled containers should be incubated for a minimum of 14 days. If two temperatures are used for incubation of media filled samples, then these filled containers should be incubated for at least 7 days at each temperature. Following incubation, the medium-filled containers should be inspected for growth. Media filled isolates are identified by genus and, when possible, by species in order to investigate the sources of contamination.
Critical issues in performing media fills are the number of fills to qualify an aseptic process, the number of units filled per media fill, the interpretation of results, and implementation of corrective actions. Historically, three media-fill runs during initial qualification or start-up of a facility are conducted to demonstrate consistency of the aseptic processing line. The minimum number of units to demonstrate a contamination rate of not more than 0.1%, which is the criterion for acceptance of a successful media-fill run, is at least 3,000. It should be emphasized that many firms in the United States and other countries are filling more than 3,000 units in a single media-fill run.4 Pilot plant facilities used for preparing small clinical lots may use smaller media fills.
A number of international documents (i.e., ISO and EU-GMP) have also cited an expectation of zero positives out of 3,000 media filled units at the 95% confidence level. However, it is recognized that repeated media runs are required in order to confirm the statistical validity of the observed contamination rate for the process.
PDA Technical Monograph Number 17,4 “A Survey of Current Sterile Manufacturing Practices,” indicated that many manufacturers believe that their aseptic processes are capable of contamination rates below 0.1%.
Since the most critical source of contamination in the clean room is the personnel, visual documentation that can be helpful in correlating production activities to contamination events during media fills is encouraged. The widespread use of isolator systems for sterility testing has demonstrated that elimination of personnel does reduce contamination in aseptic handling.